There was a tight feeling in John Arhin’s chest. He felt short of breath in an alarming way on April 13, 2022. Before dizziness set in, the day started normally — Arhin was hanging out with his best friend. But it ended with him being admitted to Montefiore.
This feeling was different for the Allerton resident who had had his fair share of heart problems, most notably a bypass and pacer pacemaker.
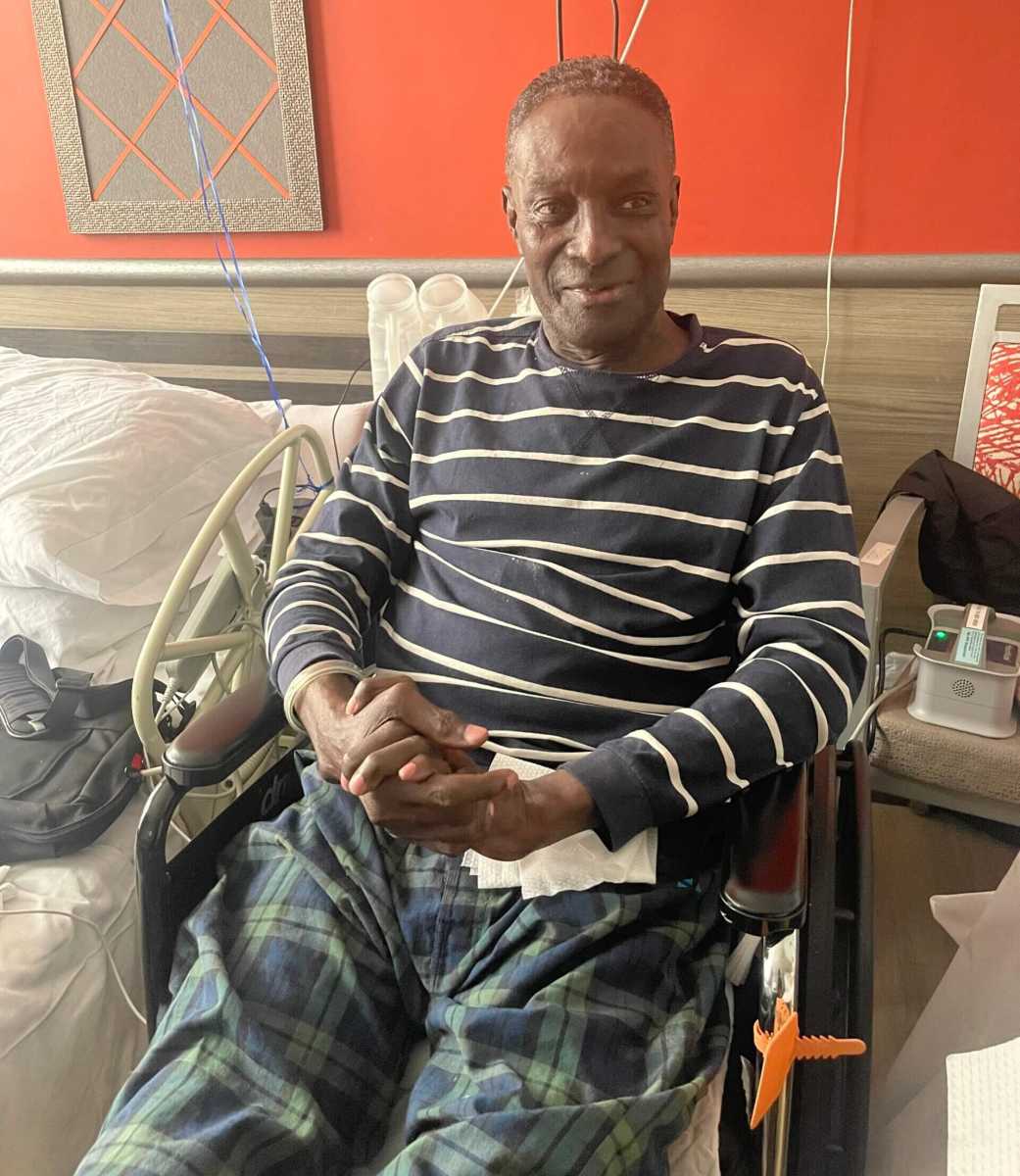
Now Arhin, 60, sits in a hospital bed at Beth Abraham Center for Rehabilitation and Nursing after a full year of experiencing the first signs of congestive heart failure. He sits on his wheelchair with his legs laid out on another chair, wearing a black– and white–striped shirt, green and navy plaid pants and beige socks. The Leeds United vs. Leicester City’s soccer game is on the TV on a sunny April afternoon.
The road to soon getting discharged wasn’t an easy one for Arhin, who didn’t know if he would see the day. He was readmitted to Montefiore ER many times over the duration of his recovery for various reasons from shocks from his implantable cardioverter-defibrillator (ICD) to an infection.
The accredited rehab center by the American Heart Association and hospital have been helpful to his healing, but Arhin knows the rest is up to him.
“I’m lucky I have good doctors that take care of me. If not by now I[‘d be] dead, gone. I’m lucky that I have somebody to help and I know what is troubling me now so there [are] certain things I won’t do,” he said.
In his original hometown of Ghana, Arhin worked on a cargo ship for 10 years where he did a lot of drinking and smoking. Life on a boat had him and his coworkers “enjoying themselves” wherever they served.
The first thing he plans to do when fully discharged is to call his best friend to go to the butcher’s shop and buy a goat head to make. Arhin also looks forward to visiting his home country.
The retired home attendant urged others to take care of their health, when speaking with the Bronx Times, after experiencing this tumultuous recovery.
“They should concentrate on their work and no more drinking and smoking. And then they should watch what they eat, ” Arhin said.
Although he is better than he felt since being admitted last year, he is aware that life will not be the same as before.
Arhin hopes that no one in his family, such as his brothers, sisters and seven kids, encounters the same heart issues he has dealt with.
The Bronx, where Arhin lives, is the worst county in New York state for health outcomes and health factors. According to the city department of health’s 2017 report, 22% of deaths from heart disease occur in adults under 65 years of age in the Bronx compared to the state average of 17%.
In 2018, 30% of New Yorkers — 1.9 million adults — suffered hypertension, which is also known as high blood pressure. Black and Latino adults are disproportionately affected by hypertension, which can increase the risk of heart disease.
This is one of the reasons Centers Health Care, which owns Beth Abraham Center, and The American Heart Association came together on April 17 for their first Bronx Hypertension Campaign event at the Centers’ corporate office. The two organizations joined forces and invited other Bronx health community institutions — Montefiore, Bronxworks and Empire BlueCross BlueShield to name a few — to collaborate and devise viable solutions to combat hypertension and by extension heart disease.

Robin Vitale, vice president of Community Impact for the American Heart Association, led the meeting by detailing the reason everyone is here today — hypertension management strategies. Vitale brought up components that have shown a decrease in hypertension, such as better nutrition through food pantries for example, and no smoking tobacco.
Sadia Choudhury, chief corporate compliance & quality assurance officer of Damian Family Care Center, with Lysna Paul, hypertension program manager for Damian, were highlighted for their success with blood pressure cuffs in the fight for hypertension. They talked about the importance of the cuffs and it’s distribution. Choudhury said they’re also looking to give patients free cuffs through a potential loaner program. Through a grant that expires soon, Damian can provide blood pressure devices and support via health and wellness company as well as Remote Patient Monitoring vendor, iHealth.
“Bringing awareness of how to improve their hypertension, and how to keep it functional after they get it to that level is an important aspect to look at when you’re looking at hypertension,” Paul said.
Brooklyn Councilmember Mercedes Narcisse, who chairs the Council’s Committee on Hospitals, couldn’t make it in person so she zoomed into the meeting momentarily, stating she is glad to be a part of this collaborative. Narcisse emphasized that high blood pressure is a silent killer that needs to be addressed. She further discussed accessibility and health equity with a bill she is working on getting passed that will “provide blood pressure machines in high-need publicly accessible areas throughout the city.”

Charmaine Browne, assistant director of the Take the Pressure Off, NYC! at the NYC Department of Health and Mental Hygiene, presented on the work the city is doing by bringing up Take the Pressure Off, NYC! . Take the Pressure Off, NYC! is the first citywide initiative for preventing and managing hypertension. Browne talked about “targeting local challenges and identifying the barriers” of hypertension that New Yorkers face especially Black and Latino New Yorkers. She also mentioned city resources such as free blood pressure monitors at health sites (NYC Health Map), health bucks and free fitness classes with Shape Up NYC.
During the roundtable discussion questions and possible solutions about access, patient retention, funding, education and engagement were brought up. Dr. Guido Macchiavello, director of Ambulatory Internal Medicine at SBH Health System, for example shared some strategies he follows for patient retention for follow-up appointments. He sends text message reminders through Doximity and also has a patient care navigator call his geriatric patients three then two days before. They’ll also rearrange schedules based on the patient’s capacity of showing up on the same day.

“The Bronx is not full of health care providers that don’t care. There’s a lot of us that care. And this collaborative, I think, will bring us together and provide a foundation for a cause that we can address collectively. I think that’s the main reason why we want the partners [here] today,” said Steve Carr, The Centers Health Care’s chief sales officer.
As the event winded down, Centers and AHA tentatively set a July date to reconvene to check in about the solutions and ideas produced during the event. Everyone is tasked with action items and a plan to see them through a 30, 60, and 90-day mark structure. Vitale said this wasn’t a one-time event, they want to grow and make it a regular occurrence.
“This is an ongoing conversation and we want to invite anyone that has an interest in helping us on this effort to join us. This is deeply focused on building out biosystemic solutions. So we’re gonna need everyone’s help to address those concerns,” she said.
Reach Demetria Osei-Tutu at oseitutud13@gmail.com. For more coverage, follow us on Twitter, Facebook and Instagram @bronxtimes